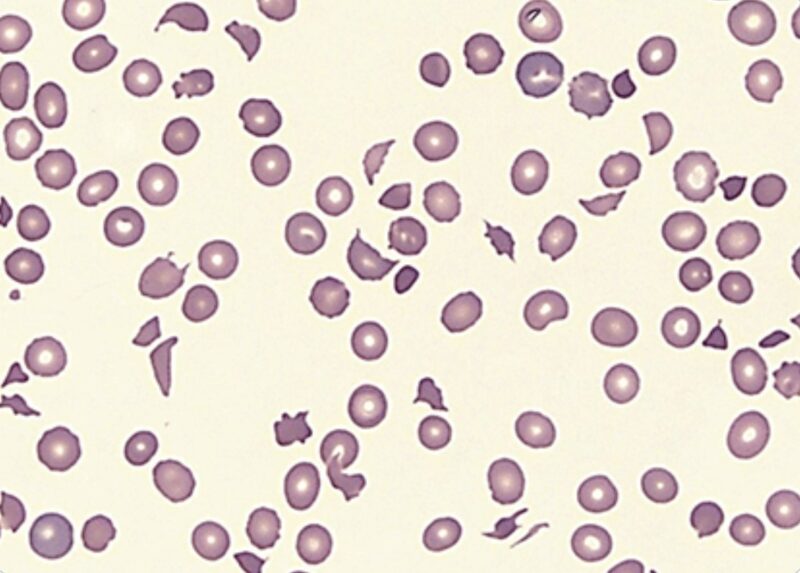
Microangiopathic Hemolytic Anemia (MAHA) represents a group of disorders characterized by the mechanical destruction of red blood cells due to passage through small, occluded blood vessels.
This condition is often accompanied by thrombocytopenia without coagulation pathway defects.
Hemolytic Uremic Syndrome (HUS) and Thrombotic Thrombocytopenic Purpura (TTP) are the primary diseases within the MAHA spectrum, caused by various etiological factors but manifesting through a common pathological mechanism.
Key Takeaways
- MAHA involves the destruction of red blood cells due to passage through damaged blood vessels.
- It’s often accompanied by thrombocytopenia and diagnosed through specific lab findings.
- TTP and HUS are primary diseases within the MAHA spectrum, each requiring distinct treatments.
- Emerging therapies like caplacizumab and gene therapy offer new hope for MAHA patients.
- Early diagnosis and treatment are crucial for managing MAHA and preventing severe complications.
Etiology and Pathogenesis
MAHA arises from several causes, including infections (notably by Shiga Toxin-producing E. coli), genetic mutations, autoimmune disorders, certain medications, and cancers. These factors lead to endothelial damage and platelet aggregation, forming microthrombi that obstruct microcirculation and shear red blood cells. This process underpins the hemolysis observed in MAHA.
Diagnostic Insights
- Thrombocytopenia: A hallmark of MAHA, thrombocytopenia involves a reduced platelet count, often detected through a complete blood count (CBC). Platelet counts below the normal range (150,000 to 450,000 platelets per microliter) suggest platelet consumption within the microcirculation, a critical indicator of MAHA.
- Schistocytes on Peripheral Smear: The presence of schistocytes, or fragmented red blood cells, in a peripheral blood smear is a diagnostic cornerstone for MAHA. These fragments result from the mechanical shearing of erythrocytes as they pass through occluded microvasculature. The identification of schistocytes requires a manual review of the smear by a trained hematologist or pathologist.
- Normal Coagulation Tests (PT/PTT): Prothrombin time (PT) and partial thromboplastin time (PTT) assess the blood’s clotting ability. In MAHA, unlike in disseminated intravascular coagulation (DIC), these tests usually return normal results. Normal PT/PTT in the presence of hemolytic anemia and thrombocytopenia helps in ruling out coagulopathies and directing the diagnosis towards MAHA.
Emerging Diagnostic Tools and Biomarkers
Recent advancements have introduced new diagnostic tools and biomarkers that improve the specificity and sensitivity of MAHA diagnosis:
- ADAMTS13 Activity Assay: Particularly relevant in Thrombotic Thrombocytopenic Purpura (TTP), one of the subtypes of MAHA, this assay measures the activity of the ADAMTS13 enzyme. Severely reduced or absent enzyme activity, often alongside the presence of inhibitory antibodies against ADAMTS13, confirms the diagnosis of TTP.
- Genetic Testing: For atypical Hemolytic Uremic Syndrome (aHUS), another MAHA subtype, genetic testing can identify mutations in genes involved in the complement system. These genetic insights are crucial for confirming the diagnosis and tailoring treatment strategies, particularly with the use of complement inhibitors.
- Lactate Dehydrogenase (LDH) Levels: Elevated LDH levels in the blood signify increased cell turnover and hemolysis, supporting the diagnosis of hemolytic anemias, including MAHA.
- Haptoglobin Levels: Haptoglobin, a protein that binds free hemoglobin, is typically reduced in hemolytic conditions. Low haptoglobin levels further support the presence of hemolysis.
- Direct Antiglobulin Test (DAT): While typically negative in MAHA, a DAT test can help exclude autoimmune hemolytic anemias, where the body’s immune system mistakenly attacks its own red blood cells.
Clinical Management
Current Therapies
Treatment strategies for MAHA, particularly TTP and HUS, have evolved significantly:
- TTP: Plasma exchange remains the cornerstone of TTP treatment, removing autoantibodies against ADAMTS13 and replenishing functional ADAMTS13. Additionally, immunosuppressive therapies are used to reduce antibody production.
- HUS: Management focuses on supportive care, including hydration and renal support. In STEC-HUS, antibiotics are generally avoided due to the risk of toxin release. Eculizumab, a complement inhibitor, has shown promise in atypical HUS by targeting the complement pathway involved in endothelial damage.
Advancements in Treatment
Recent advancements have introduced new therapeutic agents targeting specific pathways implicated in MAHA:
- Caplacizumab: A humanized monoclonal antibody that blocks von Willebrand factor (vWF) interaction with platelets, reducing platelet aggregation and thrombus formation, has been approved for treating TTP.
- Gene Therapy: Experimental approaches are exploring gene therapy for hereditary forms of HUS, aiming to correct underlying genetic defects.
FAQ
What are the common symptoms of MAHA?
Common symptoms include fatigue, weakness, shortness of breath, dark urine, jaundice, and an enlarged spleen. These symptoms result from the underlying anemia and hemolysis characteristic of MAHA.
How is MAHA different from other types of anemia?
MAHA is specifically caused by the mechanical destruction of red blood cells as they pass through small, damaged blood vessels. This distinguishes it from anemias caused by nutritional deficiencies, bone marrow disorders, or other causes.
Can MAHA lead to long-term complications?
Yes, if untreated, MAHA can lead to severe complications such as kidney failure, severe neurological conditions, and increased risk of bleeding due to thrombocytopenia.
Is MAHA a genetic disorder?
While some forms of MAHA, like atypical HUS, can have a genetic component, not all cases are inherited. Environmental factors, infections, and other conditions can also trigger MAHA.
Can MAHA be cured?
Treatment can be highly effective, especially with early diagnosis. While some forms of MAHA may be managed rather than cured, advancements in treatment have significantly improved outcomes.
Conclusion
MAHA, encompassing conditions like TTP and HUS, challenges clinicians with its complex pathogenesis and varied clinical presentations. However, with advancements in diagnostic methods and therapeutic interventions, there is renewed hope for effective management. Continued research and innovation are critical to further unraveling the mysteries of MAHA and improving patient outcomes.