The Autonomic Nervous System (ANS) is a fascinating and intricate part of our body that plays a pivotal role in regulating involuntary functions. From the beating of our heart to the dilation of our pupils, the ANS is constantly at work, ensuring that our body responds appropriately to the ever-changing environment.
In this article, we will delve deep into the workings of the ANS, shedding light on its anatomy, functionality, and the profound impact it has on our daily lives.
The Autonomic Nervous System (ANS) is a crucial component of the peripheral nervous system. It’s responsible for the subconscious control of our visceral organs, ensuring that our body functions seamlessly without our conscious effort.
The ANS is divided into two primary subsystems: the sympathetic nervous system and the parasympathetic nervous system. These systems, while distinct in their anatomy, work in tandem to regulate the organs they innervate.
Their reciprocal regulatory functions ensure a balance in our body’s responses to various stimuli. In the subsequent sections, we will explore the basic themes of the ANS, delving into the specific features of the sympathetic and parasympathetic systems, their component neurons, and the primary classes of autonomic neurotransmitter receptors.
Sympathetic vs. Parasympathetic
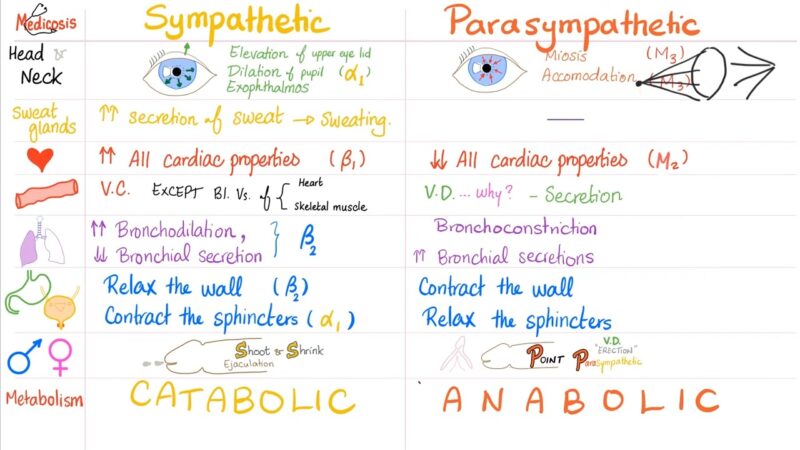
While both the sympathetic and parasympathetic systems are integral parts of the ANS, they often have opposing effects on the organs they regulate. For instance, while the sympathetic system prepares the body for “fight or flight” responses, the parasympathetic system is often associated with “rest and digest” functions.
Understanding the interplay between these systems is crucial for grasping the holistic functioning of the ANS.
Basic Control
The central nervous system (CNS) plays a pivotal role in overseeing the operations of the ANS. Various centers within the CNS contribute to this control, ensuring that the ANS functions optimally.
Role of the Hypothalamus
The hypothalamus, a small region at the base of the brain, is perhaps the most significant control center for the ANS. It integrates information from various parts of the brain and coordinates the body’s responses. While the ANS can function without higher cortical centers, the cortex can influence its output, modulating responses based on external stimuli and internal states.
Other Control Centers
Apart from the hypothalamus, other vital loci within the spinal cord and brain stem contribute to the regulation of the ANS. These centers ensure that the ANS responds appropriately to various physiological needs, from maintaining homeostasis to responding to threats.
Basic Physiological Anatomy
The ANS’s anatomy is intricate, with pathways connecting the CNS to various organs. Understanding this anatomy is crucial for grasping the system’s functionality.
Two-Neuron Systems
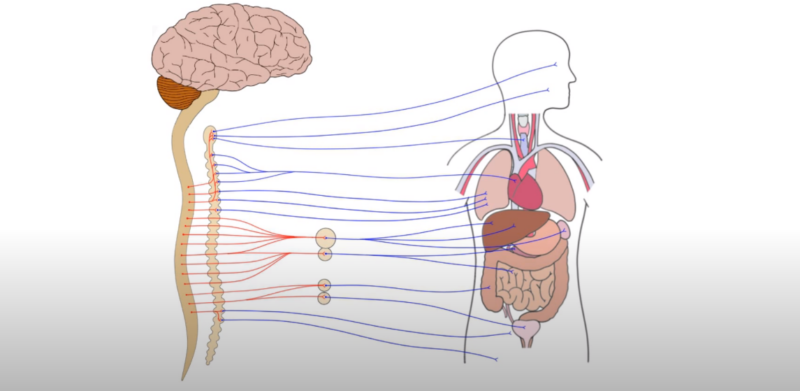
All autonomic pathways consist of two-neuron systems, distinguishing them from skeletal motor pathways. The first neuron, known as the “Preganglionic Neuron,” originates in the CNS. Its axons synapse with the second neuron, the “Postganglionic Neuron,” located outside the CNS in the autonomic ganglia.
This neuron then innervates the target organ. However, the locations of these neurons differ between the sympathetic and parasympathetic systems, leading to variations in their lengths and functions.
Neurotransmitters and Receptors
Neurotransmitters play a pivotal role in the ANS’s functioning. Preganglionic neurons in all autonomic ganglia secrete acetylcholine (Ach), which binds to nicotinic receptors on postganglionic neurons.
This binding is excitatory and results in the firing of postganglionic neurons. However, the neurotransmitters secreted by post-ganglionic neurons differ between the sympathetic and parasympathetic systems, leading to varied responses in target organs.
Basic Functionality
The ANS is not just a passive system that waits for external stimuli to react. It is an active regulator, ensuring that our body’s internal environment remains stable and balanced, irrespective of external changes.
Regulation of Visceral Functions
The ANS plays a pivotal role in controlling a myriad of visceral functions without our conscious intervention. Almost all major organs receive innervation from autonomic fibers, and in most instances, both the sympathetic and parasympathetic pathways are involved. The effects these systems exert on any particular organ can vary, but they often have opposing physiological impacts.
Sympathetic and Parasympathetic Tone
It’s essential to understand that the sympathetic and parasympathetic systems are not dormant during resting states. They maintain a baseline “tone” at all times. This means that the control of an organ isn’t just about activating one pathway over the other. It involves increasing the activity of one while simultaneously inhibiting the baseline activity of the other, ensuring a balanced response.
Specific Functionality
To truly appreciate the ANS’s impact, it’s crucial to understand the specific effects it has on various organs. These effects can be both broad and nuanced, showcasing the system’s complexity.
Effects on the Eye
The ANS plays a significant role in regulating our eyes’ responses to different stimuli:
- Sympathetic: It causes the dilation of the pupil, preparing the eye for situations that require heightened alertness.
- Parasympathetic: It contracts the pupil and promotes the lens’s convexity, aiding in close-up vision and restful states.
Regulation of Glandular Secretions
Glands across our body are influenced by the ANS, determining the amount and type of secretions they produce:
- Sympathetic: While it inhibits secretion from most glands by inducing vasoconstriction, it paradoxically increases secretion from sweat glands, aiding in thermoregulation.
- Parasympathetic: It stimulates secretion from various glands, including nasal, lacrimal, salivary, and intestinal glands, ensuring that these organs function optimally.
Influence on the GI System
The gastrointestinal (GI) system, responsible for digestion and nutrient absorption, is significantly regulated by the ANS:
- Sympathetic: It reduces peristalsis (the movement of food through the intestines) and increases the tone of sphincters, slowing down the digestive process.
- Parasympathetic: It promotes peristalsis and reduces sphincter tone, facilitating digestion and the movement of food.
Cardiac Regulation
The heart, being the central pump of our circulatory system, is under the meticulous regulation of the ANS. This ensures that our heart rate and contractility adjust according to our body’s needs, whether we’re resting or engaging in strenuous activity.
Sympathetic Influence on the Heart
The sympathetic system acts as the accelerator for the heart:
- Sympathetic: It increases both the heart rate and the force of contraction. This ensures that during times of stress or physical exertion, our muscles and organs receive an adequate supply of oxygenated blood.
Parasympathetic Influence on the Heart
The parasympathetic system, on the other hand, acts as a brake:
- Parasympathetic: It decreases the heart rate and the force of myocardial contraction. This is crucial during restful periods, ensuring that the heart doesn’t overwork and conserves energy.
Vascular Regulation
The ANS plays a pivotal role in regulating the tone of our blood vessels, which in turn affects blood pressure and blood flow to various organs.
Sympathetic Control of Vasculature
The sympathetic system has a more pronounced effect on our blood vessels:
- Sympathetic: It promotes vasoconstriction, increasing the total peripheral resistance. This can raise blood pressure. Additionally, it induces vasoconstriction, enhancing the preload on the heart, which can increase cardiac output.
Parasympathetic Influence on Vasculature
The parasympathetic system has a limited direct effect on most of our vasculature:
- Parasympathetic: It has minimal direct influence on blood vessels. However, its indirect effects, especially through the release of nitric oxide, can lead to vasodilation in specific vascular beds.
Renal Regulation
The kidneys, responsible for filtering our blood and maintaining electrolyte balance, are also under the ANS’s influence.
Sympathetic Regulation of the Kidneys
The sympathetic system plays a role in water and salt balance:
- Sympathetic: It promotes salt retention, which can lead to water retention. This is crucial during situations where the body might be at risk of dehydration or when blood volume needs to be preserved.
Final Words
The Autonomic Nervous System, often operating behind the scenes, is a testament to the body’s intricate design and its ability to adapt and respond to myriad challenges. From regulating our heartbeat to ensuring our pupils adjust to changing light, the ANS is a silent guardian that works tirelessly.
As we’ve journeyed through its functionalities and influences, it becomes evident that understanding the ANS is not just for medical professionals but for anyone curious about the marvels of the human body. It reminds us of the delicate balance and interplay of systems that keep us alive, thriving, and capable of experiencing the world around us.